How Long Will Symptoms Of Dizziness Last Following COVID-19 Infection? How To Remove Long-Term COVID Dizziness?
- Long Covid Classified Treatment Options
- 28 Oct, 2022
Summary
Numerous studies have confirmed that novel coronavirus infection in humans produced long-lasting side effects even after the symptoms of the initial infection disappeared completely, which we call long-term COVID-19 symptoms. These post-coronavirus remnants mainly were the appearance of brain fog, fatigue, shortness of breath, chronic pain, loss of smell, loss of taste, early symptoms Parkinsonism-like, early symptoms of Alzheimer 's-like disease and diarrhea. These long-term COVID-19 symptoms can put eternal side effects on the body.
According to published medical research papers, long-term COVID-19 symptoms are mainly caused by the damage to the body's own immune system and inflammation following COVID-19 infection. Studies have also shown that for a small proportion of patients with COVID-19, as trace amounts of coronaviruses remain latent in their bodies for a long time, this residual trace amount of live virus will continue to invade the body's cells and repeatedly activate the immune system, leading to long-term inflammatory response. This long-term effect is concentrated in the heart, kidneys, and brain, in addition to being manifested in the lungs.
The author found a large number of people with long-term COVID-19 symptoms of dizziness by studying Long COVID-related medical research papers. This article summarized the long-term COVID dizziness and gave in-house self assessment to judge whether people developed these symptoms. Then, the pathogenesis of dizziness caused by long-term COVID-19 was analyzed from the perspective of trace COVID-19 residues, and the therapeutic ideas of western medicine for the dizziness after infection with COVID-19 were given.
Due to the limitation of western medicine treatment against long COVID-19 symptoms of dizziness, this paper also recommended some traditional Chinese medicine, including Chinese medicine formula and acupuncture treatment, to treat the symptoms of dizziness. In addition, this paper made advises patients with long-term COVID-19 dizziness on taking healthcare products, as well as on exercise, diet, and sleep. In the end, we hope that the treatment program for long-term COVID-19 symptoms of dizziness suggested in this paper could benefit patients by improving their symptoms as soon as possible, and even cure these symptoms of dizziness caused by novel coronavirus.
Keywords: Long COVID, Post-COVID Conditions, long COVID dizziness, symptoms of dizziness after COVID-19 infection, dizziness induced by COVID-19
1.What Are The Manifestations Of Long-Term Covid-19 Symptoms Of Dizziness?
A large proportion of long-term COVID-19 symptoms are associated with neurological symptoms, and some medical communities use a folk colloquial vocabulary” brain fog” to facilitate the unified classification and description of post COVID-19 symptoms associated with the brain. Brain fog has not previously been regarded as a medical or scientific term, but rather a colloquial description of a state in which people cannot think normally and clearly when they develop influenza or other diseases. Ordinary people use the fog in their brains to describe problems arising in their usual cognition or thinking, such as dizziness, tinnitus, difficulty in concentrating, memory loss, slower thinking speed, inability to think keenly without creativity, and difficulty in formulating plans.
During rehabilitation following COVID-19 illness, many patients said they experienced "brain fog". According to figures given in the study report, about 10% of patients infected with COVID-19 will experience long-term COVID-19 symptoms. At present, it has become customary in the medical community to classify the symptoms of dizziness and tinnitus caused by COVID-19 infection as long COVID brain fog. According to the statistics in the study report, up to 60% of patients with long-term COVID-19 had some degree of dizziness or vertigo, and up to 30% had some degree of tinnitus. And dizziness, vertigo, tinnitus, the three symptoms have a very high degree of coincidence.
According to the published medical papers on the symptoms of long-term COVID-19 of dizziness, we concluded clinical manifestations of dizziness as follows:
(1) Dizziness: feel a false sense of movement or rotation, vertigo, feel lightheaded, unstable to stand or walk, and likely to lose balance and fall.
(2) Blurry vision: blurred vision is found in the morning, and if look at the computer and mobile phone screen for a slightly longer time, feel that vision is trance and eyes are tired.
(3) Tinnitus: refers to the condition in which the external environment does not make a sound, but feels to hear a certain noise, feels that the ear is blocked by cotton, over-high internal pressure,buzzing,and it’s easy to be anxious or difficult to concentrate.
(4) Common accompanying symptoms, brain fatigue: feel drowsy, it’s easy for brain to feel tired, feel fatigued when thinking,it’s easy to feel sleepy when reading, feel sleepy in the daytime.
Common accompanying symptoms, chronic headache: feel symmetrical chronic headache bilaterally on the head; often feel hot on the head and tightness on the head.
Inner ear problems that lead to dizziness (vertigo) are usually related to the person's brain, eyes, inner ear, sensory nerves, which are input systems for the sense of balance in the human body.
(1) Brain is used to automatically calculate the sense of balance of the human body.
(2) Eyes help people determine the position of the body in space and its mode of movement.
(3) Sensory nerves send information to the brain about the motor state and position of various parts of the body.
(4) Inner ears with built-in sensor can detect gravity and anteroposterior movement.
Vertigo is an illusion that makes you feel as if surroundings are spinning or moving. When suffering from inner ear disease, your brain receives signals from the inner ear that are different from those received by your eyes and sensory nerves. Vertigo is the result of your brain dealing with confusion. The usual causes of vertigo are the following:
(1) Benign paroxysmal positional vertigo (BPPV). The disease leads you to have a strong and brief illusion that you are rotating or moving. Seizures are caused by rapid changes in head movement, such as turning over in bed, sitting up, or getting a heavy blow to your head. BPPV is the most common cause of vertigo.
(2) Infection. A viral vestibular nerve infection called vestibular neuritis can cause severe persistent vertigo. If you also have sudden hearing loss, you may have labyrinthitis.
(3) Meniere 's disease. This disease presents with excessive accumulation of fluid in the inner ear. It is characterized by a sudden onset of vertigo that lasts for hours. You may also have fluctuating hypoacusis, tinnitus, and blockage of your ears.
(4) Migraine. Even people who have migraines do not have severe headaches, they may experience vertigo or other types of dizziness. Such episodes of vertigo may last from minutes to hours and may be associated with headache and sensitivity to light and noise.
Causing dizziness is also associated with problems with your body's blood circulation system, and if your heart does not pump enough blood to your brain, you may feel dizzy, weak, or unable to maintain balance. For example:
(1) Blood pressure decreased. A sharp drop in systolic blood pressure (the larger of your blood pressure reading) can cause a brief feeling of dizziness or lightheadedness. This may occur when sitting up or standing up too quickly. This condition is called orthostatic hypotension.
(2) Poor blood circulation. Cardiomyopathy, heart attack, irregular heartbeat, and transient ischemic attack can all cause dizziness. In addition, decreased blood flow may lead to insufficient blood supply to the brain and inner ear.
Causing dizziness is also associated with problems with the nervous system of the body, such as the following:
(1) Neurological disorders. Neurological conditions such as Parkinson's disease and multiple sclerosis may lead to progressive loss of balance, then cause dizziness.
(2) Drugs. Certain medications (such as antiepileptics, antidepressants, sedatives, and tranquilizers) may cause side effects such as dizziness. In particular, blood pressure medications can cause fainting if blood pressure drops too low.
(3) Anxiety disorder. Certain anxiety disorders cause lightheadedness or dizziness, often called dizziness. These disorders include panic attacks and fear of leaving home or staying in an empty large square (agoraphobia).
(4) Low iron content (anemia). If anaemic, dizziness may occur with other signs and symptoms, including fatigue, weakness, and pallor.
(5) Low blood glucose levels (hypoglycemia). This condition usually occurs in diabetic patients taking insulin. Dizziness (lightheadedness) may be accompanied by sweating and anxiety.
(6) Carbon monoxide poisoning. Symptoms of carbon monoxide poisoning are usually described as "flu-like" and include headache, dizziness, weakness, stomach discomfort, vomiting, chest pain, and confusion.
(7) Overheating and dehydration. You may get dizzy from overheating (hyperthermia) or dehydration if you join activities or drink too little water in hot weather. This is especially true when you take certain heart medicines.
In this paper, from the perspective of COVID-19 infection, we simply analyze why COVID-19 infection will cause a large number of people suffering from long-term COVID dizziness, vertigo and tinnitus.
2.How Long Will Symptoms Of Dizziness Last Following Covid-19 Infection?
2.1 What are Post Covid-19 Symptoms of brain fog?
According to the definition of the World Health Organization, Post-COVID Conditions or Long COVID, also known as Post COVID-19 syndrome, refers to since the patient was infected with the novel coronavirus, the results of his PCR showed positive as criteria, and he still suffers uncomfortable symptoms after 3 months. More detailed updated statistical information on the incidence of Post Covid-19 Symptoms according to the timeline can be found in the figure below.
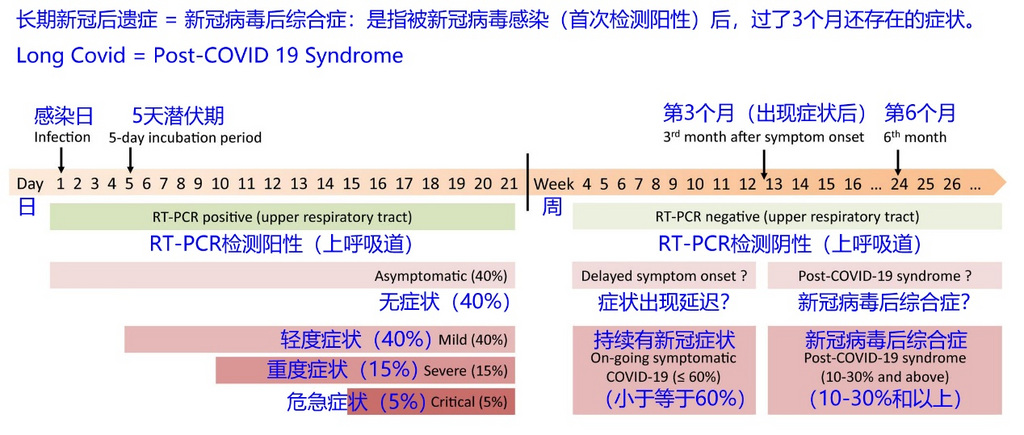

Post-COVID Conditions are mainly concentrated in five aspects, including respiratory syndrome, cognitive system syndrome, chronic fatigue syndrome, chronic pain syndrome, and mental syndrome, such as long-term COVID-19 brain fog, which belongs to the cognitive system syndrome. Long-term COVID chronic fatigue are one of chronic fatigue syndrome.
If you have a history of the novel coronavirus, which means your previous result of PCR test showed positive, and before infection with the novel coronavirus, you didn’t suffer from dizziness, but now you are presenting these symptoms of chronic dizziness in the above section, you are likely to afflict by Post Covid-19 Symptoms of dizziness.
2.2 How long will symptoms of dizziness last following COVID-19 infection?
During the acute phase of COVID-19 infection, dizziness caused by the onset of COVID-19 infection usually last 10 to 14 days. But even after recovery from acute symptoms early in COVID-19 infections, people still feel dizziness. A study found that more than half of people still experience daily chronic dizziness for up to six months after illness.
In 2021, in a study designed to describe long-term COVID-19 symptoms in more than 3,000 people from 56 countries, researchers found that 88% of respondents represented neurological symptoms such as cognitive, dizziness and memory problems. During the first few months after the onset of COVID-19 symptoms, these symptoms showed an increasing trend and then started to decrease gradually. At the beginning of the 7th month after the onset of COVID-19, 55.5% of respondents reported suffering from cognitive problems such as brain fog.
A 2022 study investigated the rehabilitation of individuals with neurological symptoms such as long COVID brain fog and dizziness. The mean duration of brain fog since participants developed symptoms of COVID-19 infection was 14.8 months. After an initial evaluation, participants were followed up for 6 to 9 months. During follow-up, no significant changes were observed in the reporting of brain fog symptoms compared with the initial assessment, which means there were no significant change among most patients with brain fog. Researchers still pointed out that quality of life measures of study participants remained lower than that of the general population.
According to published medical statistics papers on long-term COVID brain fog, the symptoms could last for quite a long time. The symptoms of brain fog tends to peak within a few months of infection with COVID-19 and them generally begins to improve over time. However, brain fog may still persist for several months. Recent studies have found that brain fog symptoms may last more than a year after infection with COVID-19. Moreover, studies have shown that more than 20% of patients with long-term COVID-19 symptoms of brain fog still did not get an improvement for their symptoms after a year.
In summary, the symptoms of dizziness following COVID-19 infection in the acute phase, which means in the initial stage of infection, will last for about two weeks. If you recover completely from the acute phase, the dizziness goes away. If you go through the acute phase, but there is still immune system confusion and chronic inflammatory response in the body, dizziness symptoms may last for more than a year. If there are still traces of COVID-19 in your body, the remaining virus is active from time to time to invade somatic cells, continuously destroying the immune system and causing chronic inflammation. As a result, dizziness symptoms may exist for a longer time.
3.How Does The COVID-19 Invade The Heart, Kidneys, And Brain Of The Human Body?
3.1 The process of the human immune system eliciting an inflammatory response in order to eliminate the novel coronaviruses
The response of the human immune system to the site of novel coronavirus infection is divided into two stages. In the preliminary stage, the immune system mobilizes macrophages and polymorphonuclear phagocytes (e.g., neutrophils, basophils, eosinophils) to rapidly reach the site of infection to control infection. In the following stages, the immune system of the human body takes about 4 days to establish adaptive immune mechanisms through learning, including T cell-mediated immune mechanisms to solve the infection, and the production B system-mediated antibody to clear the pathogen- the novel coronavirus, so as to prevent reinfection.
The following figure shows the process of the human immune system eliciting an inflammatory response in order to eliminate the novel coronaviruses:
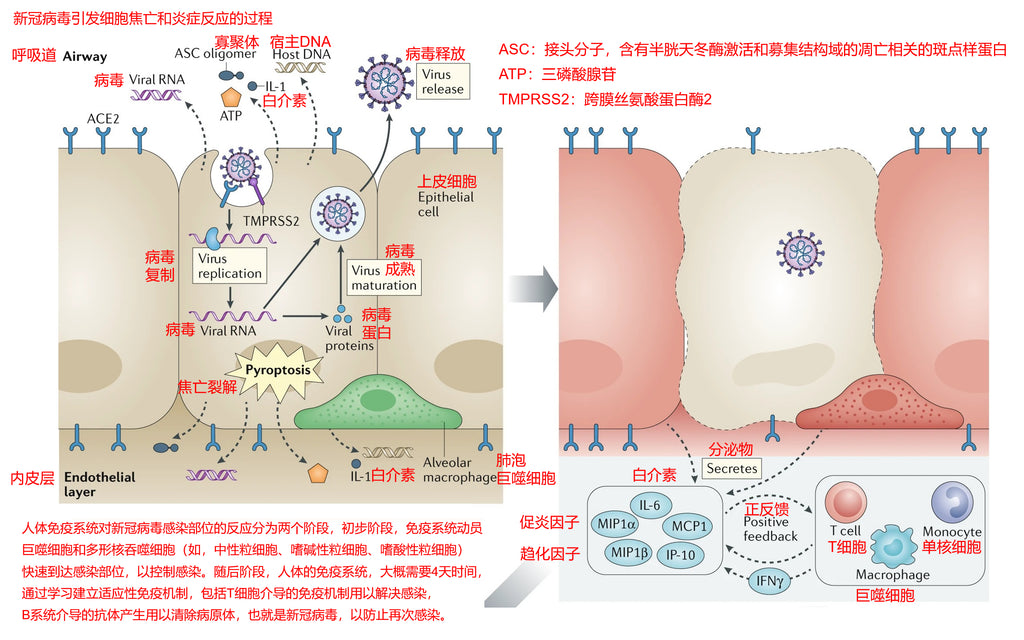
(1) Novel coronavirus enters through the respiratory tract and attaches to epithelial cells of the upper respiratory tract and lungs. The novel coronavirus recognizes host receptors via the spike glycoprotein (S protein) of coronavirus.
(2) Then the coronavirus binds to ACE2 (angiotensin-converting enzyme 2) receptor and TMPRSS2 (transmembrane serine protease 2) receptor to enter host cells in a membrane-fused manner.
(3) Novel coronavirus triggers DAMPS (Damage-associated molecular pattern) in cells leading to pyroptosis, after which cells release various factors, including ATP (adenosine triphosphate), nucleic acids, and ASC oligomers (adaptor molecules, apoptosis-associated speck-like protein with a caspase-recruitment domain).
(4) DAMPS (Damage-associated molecular pattern) is recognized by adjacent epithelial cells, endothelial cells, and alveolar macrophages. This in turn triggers the production of pro-inflammatory cytokines and chemokines including IL-6, IP-10, macrophage inflammatory protein 1α (MIP1α), MIP1β, and MCP1.
(5) These pro-inflammatory cytokine proteins attract monocytes, macrophages, and T cells produced by the immune system to the site of infection and then these cells begin to perform their duties to eliminate the novel coronavirus.
(6)At the same time, T cells will produce IFNγ in large amounts and establish a pro-inflammatory feedback loop. Pyroptosis also generates G-CSF (granulocyte colony-stimulating factor) and TNF (tumor necrosis factor).
(7) Immune cells accumulate further at the site of infection, resulting in excessive production of pro-inflammatory cytokines and further damage of the cellular environment at the site of infection, thus promoting a further inflammatory response.
There are trace viruses that escape in the human body in the long term, which will persistently infect and invade human tissue cells, causing tissue damage. Tissue damage, in turn, triggers chronic inflammation. This chronic inflammation is produced by a persistent immune response, also causing persistent massive cytokine diffusion. The continuous breakdown of a large number of cytokine proteins can lead to autoimmunity. Autoimmunity refers to the immune response produced by organisms against healthy cells and tissues of their bodies. Any disease caused by this immune abnormality is called autoimmune disease.
The persistence of trace novel coronavirus continues to deteriorate the situation, leading to T cell failure and immune memory defects. Defects in immune memory can make the immune system gradually insensitive to immune pathways that eliminate novel coronavirus, eventually becoming a coexisting state. This condition is characterized by generalized diffuse chronic inflammation. In the long run, the function of body organs and tissues is reduced.
Because novel coronavirus can easily mutate, so far as more and more coronavirus variants appear and the ability of immune escape is increasing, this makes the effect decrease when the antigens (HLA) produced by the human immune system to clear novel coronavirus, which means there will be a small number of novel coronavirus immune escape. Novel coronavirus in some patients has not yet been completely cleared, but because the human immune system is suppressing these coronaviruses, leading the content of novel coronavirus too small so as to make PCR tests negative.
3.2 The process of COVID-19 invading the heart and kidneys along the blood circulation system
According to published research papers on long-term COVID-19 symptoms, we conclude that human body with novel coronavirus infection has been affected with the following manifestations:
(1)First, because novel coronavirus can easily mutate, so far as more and more coronavirus variants appear, and the ability of immune escape is increasing, this makes the effect decrease when the antigens (HLA) produced by the human immune system to clear novel coronavirus, which means there will be a small number of novel coronavirus immune escape. Novel coronavirus in some patients has not yet been completely cleared, but because the human immune system is suppressing these coronaviruses, leading the content of novel coronavirus too small to make PCR tests negative.
(2)For patients infected with novel coronavirus, the virus also invades the cardiovascular system of the human body and spreads to various organs and tissues of the human body with blood circulation. Studies have shown that in addition to the acute phase of infection with novel coronavirus, coronavirus will directly pass through the ACE2 receptor expressed on vascular endothelial cells and myocardial cell membranes entering the cardiovascular system, cause cells damage. Some residual coronaviruses in body will also accumulate in interstitial cells and resident macrophages in the heart for a long time. These small residual coronavirus lead the PCR testing is negative and will produce persistent damage to pericardial tissue. And this persistent damage to the heart can lead to unstable blood pressure conditions, which can easily cause dizziness.
(3)The persistence of trace novel coronavirus continues to deteriorate the situation, leading to T cell failure and immune memory defects. Defects in immune memory can make the immune system gradually insensitive to immune pathways that eliminate novel coronavirus, eventually becoming a coexisting state. This condition is characterized by generalized diffuse chronic inflammation. In the long run, the function of body organs and tissues is reduced.
(4)The kidney plays an important role in filtering blood and removing harmful substances from blood, and is an important organ to reduce the inflammatory response of the human body. The kidneys are essential to maintain a healthy balance of water, salt and minerals in the blood, which allows nerves, muscles and other tissues in other parts of our body to function properly. Kidney is a critical organ of human metabolism, studies have shown that kidney is the key factor to maintain the normal operation of human immune system, human health and anti-aging. After the COVID-19 epidemic, researchers found that a small amount of residual live coronaviruses would also be hidden in the interstitial cells and resident macrophages of the kidney for a long time, and active from time to time, causing chronic damage to the kidneys. This condition leads to aging of kidney function, which in turn reduces the function of the body's immune system.
(5)For patients infected with novel coronaries, some people experienced the virus breaking through the blood-brain barrier and invading nerve cells in the brain. Evidence has been found that novel coronavirus triggers neuroinflammation and neurodegeneration in the brain. This condition can further cause metabolic abnormalities in the brain, such as capillary microthrombi in the brain, nerve cell hypoxia in brain, and so on, which may be one of the causes of long COVID cognitive dysfunction.
3.3 The process of novel coronavirus invading the brain through the olfactory nervous system and leading to brain inflammation
Studies have shown that the coronavirus can trigger inflammation of the olfactory bulb or even atrophy of the olfactory bulb if it further invades epithelial cells in the olfactory bulb, such as capillary epithelial cells, which disrupts the transmission of electrical signals between olfactory neuron cells and mitral neuron cells. If the virus further invades the olfactory brain, it is the part of the limbic system responsible for the logical processing of encoding and decoding olfactory electrical signals. This makes the electrical signals of the olfactory nervous system unable to be normally understood and operationalized by the brain, which is one of the causes of cognitive dysfunction.
The following figure shows how the novel coronavirus invades the brain through the olfactory nervous system and leads to brain inflammation:
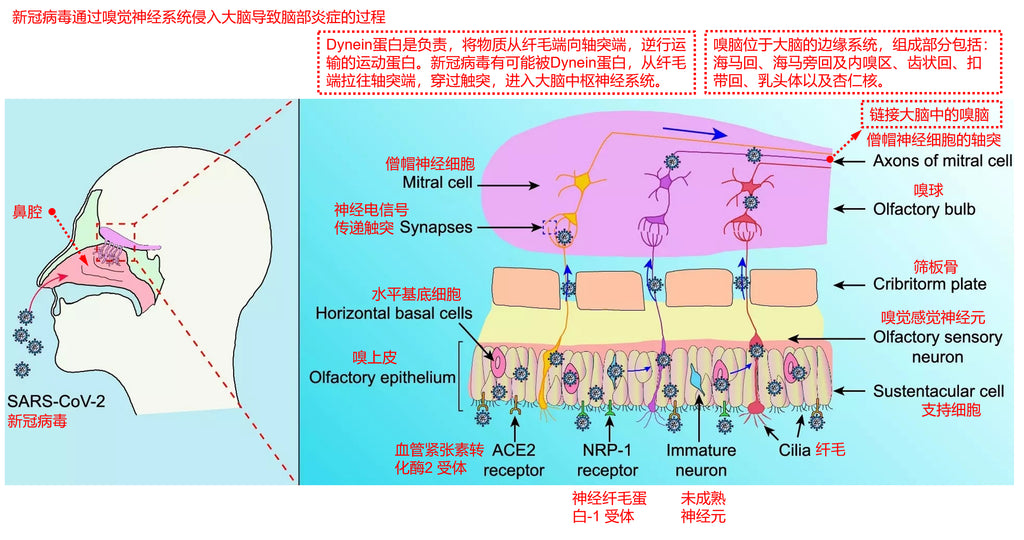
(1) Novel coronavirus enters through the respiratory tract and attaches to epithelial cells of the upper respiratory tract and lungs. The novel coronavirus recognizes host receptors via the spike glycoprotein (S protein) of coronavirus.
(2) It then binds to ACE2 (angiotensin-converting enzyme 2) receptor and TMPRSS2 (transmembrane serine protease 2) receptor and enters Sertoli cells of the olfactory epithelium and horizontal base cells of the olfactory epithelium in a membrane-fused manner.
(3) Extracellular vesicles (EV) are nanoscale membrane vesicles composed of lipid bilayers and secreted by all cell types. They act as carriers, protecting macromolecules such as proteins and RNAs from enzymatic degradation, and transporting these macromolecules between different cells, from adjacent cells to more distant cells, or immune cells. In addition, specific extracellular vesicles (EVs) have been shown to be able to cross the brain barrier.
(4) Very small amounts of novel coronavirus in Sertoli cells of the olfactory epithelium and horizontal base cells of the olfactory epithelium may be encapsulated into extracellular vesicles (EVs) and then enter olfactory neuronal cells.
(5) In neuronal cells, Dynein protein is the motor protein responsible for retrograde transport of substances from the cilia end to the axons end. The novel coronavirus is likely to be pulled from the cilia end of olfactory neurons to the axonal end by the Dynein protein, thereby entering the olfactory bulb.
(6) In the olfactory bulb, olfactory neurons and mitral neurons communicate neuroelectrical signals through touch process connections, at which time novel coronavirus may be encapsulated into extracellular vesicles (EVs) and then into mitral neuron cells.
(7) In mitral neurons, novel coronavirus may be retrogradely transported by Dynein protein into deeper brain neurons and thus enter the central nervous system of the brain.
The brain region connecting the olfactory bulb is called the limbic system of the brain, also known as the olfactory brain. If the virus further invades the olfactory brain, which is the part of the limbic system of the brain that is responsible for the processing of logic operations for the encoding and decoding of olfactory electrical signals, this makes the electrical signals of the olfactory nervous system unable to be normally understood and operated by the brain, which is the cause of cognitive dysfunction and also one of the causes of brain fog symptoms.
3.4 The process of novel coronavirus invading the brain through the blood-brain barrier or the parenchyma of ventricular organs and resulting in brain inflammation
According to the current medical research results and the generally agreed consensus, there may be the following four ways for the novel coronavirus to directly invade the brain:
(1) The coronavirus invades the brain directly through olfactory organ tissues and the olfactory nervous system.
(2) The coronavirus crosses the blood vessels, breaks through the blood-brain barrier, and directly invades the brain.
(3) The coronavirus passes through blood vessels and leaks to the brain at certain weak spots in ventricular organs, where these endothelial cells are not tightly connected and also lack an astrocyte interception barrier.
(4) The coronavirus infects peripheral nerve cells in human organ tissues, and is transported retrogradely to the brain end through the Dynein protein, and then leaks to the brain by latency into extracellular vesicles (EV). This possibility has not yet been fully substantiated.
Section 3.3 of this article explains how coronavirus invades the brain through olfactory organ tissues and the olfactory nervous system. The following article then explains the process of the coronavirus invading the brain through the blood-brain barrier or the parenchyma of ventricular organs, as shown in the following figure:
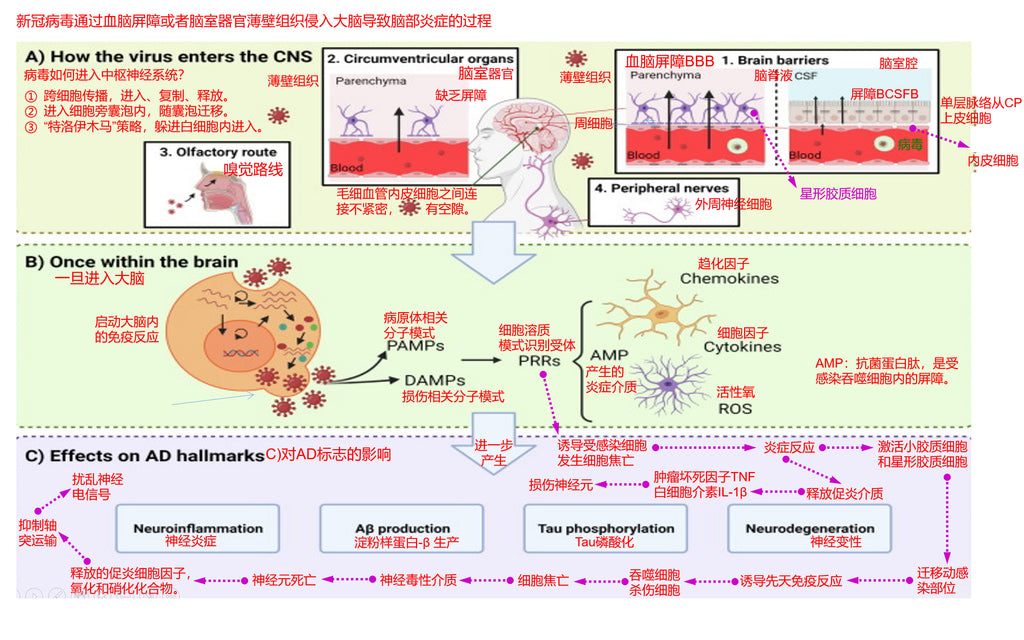
(1) The blood-brain barrier is usually composed of two modes: one is composed of an intercepting network combined of dense astrocytes, and the other is composed of a dense monolayer choroid plexus (CP) epithelial cells to form the blood-brain barrier BCSFB..
(2) The coronavirus is transported to the central nervous system through capillary blood, then infects endothelial cells of microvessels and crosses them, and then breaks through the intercepted network composed of dense astrocytes to enter the brain ventricular lumen.
(3) The coronavirus is transported to the central nervous system via capillary blood and then infects the endothelial cells of the microvessels and crosses them, then infects the monolayer choroid plexus (CP) epithelial cells and crosses them to enter the brain ventricular lumen.
(4) In addition to the blood-brain barrier, novel coronavirus enters the brain ventricular lumen from these loopholes in certain weak spots of ventricular organs, where these endothelial cells are not tightly connected and there is also a lack of astrocyte interception barrier.
(5) Once the coronavirus enters the brain, it begins to invade tissues and organs and central neuronal cells in the ventricular cavity, and start to replicat, proliferation, propagation.
(6) Viral infection activates the immune system in the brain and turns on PAMPs (pathogen-associated molecular patterns) and DAMPs (damage-associated molecular patterns), which in turn produce PRRs (cytosolic pattern recognition receptors).
(7) PRRs (cytosolic pattern recognition receptors) include: Cytokines (cytokines), Chemokines (chemokines), ROS (reactive oxygen species), AMP (antimicrobial protein peptides, which are inflammatory mediators and barrier fragments in infected phagocytes).
(8) At this point, the inflammation of the brain begins to spread.
4.What Are The Causes Of Dizziness After The Covid-19 Infection?
Vestibular system and hearing are two sensory systems mainly present in the brainstem. Auditory input is transferred from the auditory branch of the cranial nerve eight (CN VIII) to the cochlear nucleus, lateral lemniscus, inferior colliculus, and medial geniculate body, and then projects to the auditory cortex. The vestibular branch of the cranial nerve eight (CN VIII) also transmits vestibular input to the vestibular nucleus and then projects to the thalamus. Multiple thalamic nuclei contribute to vestibular processing, which contains multisensory neurons and processes vestibular, proprioceptive, and visual signals and projects to the cortex. The brainstem also controls sleep-wake cycles and vital functions through the ascending reticular activating system and autonomic nuclei, respectively.
Human inner ear structures are particularly vulnerable to ischemia and vascular injury, which can lead to hearing and balance dysfunction. Vasculitis has also been documented as one of the clinical manifestations of COVID-19. Evidence of dizziness/vertigo in patients with COVID-19 was also presented in the case report. For example, in a recent case study, a young woman infected with COVID-19 was diagnosed with acute vestibular neuritis. The disease is clinically diagnosed as vertigo and develops dramatically within minutes to hours. The patient presented with intractable vertigo symptoms associated with nausea and vomiting, probably due to stimulation or loss of emetic tracts associated with the vestibular or vestibular nuclei.
Vestibular neuritis or acute peripheral vestibulopathy is a viral or postviral inflammatory disease involving the vestibular portion of the cranial nerve eight (CN VIII). Although vestibular neuritis is generally considered a monophasic disease, multiple cranial nerve involvement may also be viral inflammation. Thus, dysfunction of the brainstem resulting from neuroinflammatory mechanisms triggered by SARS-CoV-2 can lead to sensory (including auditory and vestibular) and motor disturbances, cranial nerve palsies, disturbance of consciousness, autonomic dysfunction, etc.
The results showed that SARS-CoV-2 could attach to hemoglobin and then penetrate red blood cells. Thus, it can be transported along with erythrocytes or vascular endothelium to tissues containing ACE2 in all structures, including the brain and medulla oblongata containing large amounts of ACE2, as well as the auditory system. Previous evidence suggests that SARS-CoV-2 can spread throughout the body via the blood circulation due to ACE2, which is abundantly expressed in arterial and venous endothelial cells and arterial smooth muscle cells in many organs. Because of the attack of the coronavirus on the human vasculature, it may also disrupt the blood-labyrinth barrier and invade the inner ear structures by infected and activated monocytes. The process by which the COVID-19 of deoxygenates red blood cells also leads to hypoxia and further damage to the inner ear, causing dizziness and tinnitus.
According to the above content and the physiological structure of the balance perception system in humans, we can make inferences about the following symptoms of dizziness, and tinnitus after infection with COVID-19.
(1)COVID-19 infection leads to inflammation of the nerves in the brain, for example, it may trigger "vestibular neuritis". Viral vestibular infections can cause severe persistent vertigo. If you also have sudden hearing loss, you may have labyrinthitis.
(2) COVID-19 infection leads to inflammation of the myocardium or pericardium of the heart, which in turn leads to poor blood circulation. Conditions such as cardiomyopathy, arrhythmia, and transient ischemic attack can cause dizziness. In addition, decreased blood flow may lead to insufficient blood supply to the brain and inner ear, while producing hypoxia, but also cause dizziness.
(3) Mental problems caused by COVID-19 infection, such as insomnia, anxiety, and depression. Excessive mental stress, clearly too stressful, may lead to increased serum cortisol and epinephrine levels and decreased serotonin levels. This can sometimes cause dizziness, lightheadedness, tinnitus symptoms.
(4) COVID-19 infection leads to systemic chronic inflammation, which accelerates brain aging, for example, has the potential to trigger early symptoms of Parkinson's disease, for example, may lead to progressive loss of balance.
(5) COVID-19 infection leads to visual nerve damage, which in turn causes various visual abnormality problems, which also easily causes vertigo.
In addition to the above pathogenesis, systemic chronic inflammatory response is also considered an indirect cause of dizziness. Inflammation is a natural defense mechanism against pathogens and involves many pathogenic diseases, such as microbial and viral infections, as well as autoimmune diseases and chronic diseases. Inflammatory oxidative stress leads to excessive production of reactive oxygen species (ROS) in cells and tissues, which can damage cellular molecules such as DNA, proteins, and lipids. Reactive oxygen species (ROS) are implicated in the regulation of processes involved in cellular homeostasis and function, and are typically produced in limited amounts in vivo. Excessive reactive oxygen species (ROS) and some natural or artificial chemicals can stimulate the inflammatory process and lead to the synthesis and secretion of pro-inflammatory cytokines (e.g., interleukin 6 (IL-6), IL-1β) and tumor necrosis factor-α (TNF-α).Inflammation and oxidative stress are closely related to pathophysiological processes and to each other. Thus, activation of both processes has been found simultaneously in many pathological conditions including SARS-CoV-2 infection.
Past studies have also shown the role of reactive oxygen species (ROS) and pro-inflammatory cytokines in eliciting acute and chronic inflammation in SNHL and tinnitus, in which they may also play a role in damaging the inner ear in COVID-19 patients. Given that SARS-CoV-2 is associated with a strong systemic immune response called a "cytokine storm," excessive microglial responses may also trigger post-infectious neuroinflammation, which may also play a role in auditory glial cell injury.
5.How To Treat The Long-Term Covid-19 Symptoms Of Dizziness
At first, we need to take a thorough physical examination of our bodies, and besides taking routine examinations, we need to do another four examinations.
The first item: do several more PCR tests, nasal and throat secretions should be dipped enough to check whether the result shows positive. If it shows positive, it means there is still some active novel coronavirus in the body.
The second item: perform a neurological examination. Because neurological symptoms are highly prevalent in patients with long-term COVID, neurological testing is recommended in all patients with long COVID-19, even if some patients communicate with their physicians, they do not have neurologically uncomfortable feedback. Many patients will report "brain fog", "difficulty in concentrating" and "poor memory." Physicians should carefully evaluate the patient 's subjective symptoms on a case-by-case basis to design a patient' s neurological examination to determine pathophysiology.
Following unconventional deeper neurological tests can be performed. For example, to rule out testicular brain injury, physicians are advised to perform functional magnetic resonance imaging MRI of the brain, including functional magnetic resonance imaging MR angiography of the brain. In elderly patients, imaging findings of early abnormal brain changes in Parkinson 's disease, Alzheimer' s disease, or other types of neurodegenerative dementia can be excluded by functional magnetic resonance imaging MRI of the brain.
When patients report memory impairment, it is important to determine whether this memory impairment is caused by infection with COVID-19 or whether COVID-19 infection worsens pre-existing symptoms. If ischemic or hemorrhagic stroke is observed on functional magnetic resonance imaging MRI of brain, we must consider medical therapy to prevent recurrent stroke.
Perfusion imaging (single photon emission computed tomography) may also be performed if the patient is wealthy or if the physician suspects the diagnosis. Cerebral perfusion imaging, which is perfusion imaging using CTP and MRP, has become a routine method to examine cerebral blood flow perfusion in stroke patients. Although there is still no evidence that perfusion imaging is an essential test for stroke assessment, many centers have begun to use perfusion imaging to assess cerebral blood flow in patients.
Cerebral perfusion testing may also show the inflammation triggered by non-specific immunity (innate immunity, which refers to the normal physiological defense function congenitally possessed by the body and can make the corresponding immune response to the invasion of various pathogenic microorganisms and foreign bodies) , which is characterized by hypoperfusion in the prefrontal or temporal lobes. Although there is no established treatment for this problem, some drugs that develop brain blood may help improve the condition.
Third item: in addition to basic blood tests, we assessed thyroid hormones, zinc, ferritin, antinuclear antibodies, rheumatoid factor, and blood sedimentation rate in almost all patients. Patients with PASC may have electrolyte disturbances, anemia, thrombocytopenia, hypoalbuminemia, lipid abnormalities, and abnormal glucose metabolism. These data need to be combined with patient symptom descriptions to carefully analyze the pathogenesis behind reasoning to determine whether abnormal laboratory test results can explain the symptoms of PASC.
The fourth item: listen to the sounds of the heart and respiratory system with a stethoscope. Anemia, the signs of heart failure, latent arrhythmias such as atrial fibrillation, and pneumonitis from enteritis must be assessed when abnormal sounds are detected, or if breathlessness persists, and to check whether oxygen saturation decreases during exercise.
The following items, from item 5 to item 7, are required when the patient presents other symptoms.
Fifth item: rheumatoid arthritis or other related diseases must be analyzed when patients have symptoms of joint discomfort.
Sixth item: when the patient complains hair loss, we examine the scalp, return to the history of hair loss symptoms, and confirm the weekly amount of hair loss.
Seventh item: neuropsychological tests should also be performed if the patient has significant psychological problems.
Then, the results of the above comprehensive physical examination and four special examinations should be handed over to the doctor, and then the person should communicate with the doctor to describe one’s own long-term COVID-19 symptoms of dizziness in detail.
Additionally, the doctor can design the best treatment for you. Because the situation varied from person to person, after the interview the treatment plan given by the doctor is also different, so this paper cannot give a general treatment plan.
The rough ideas for designing the treatment plan are as follows:
(1) According to the results of the patient's comprehensive physical examination and 4 special examinations as well as the communication with the patient, find out the most likely pathogenesis of the patient's long-term COVID symptoms of dizziness, vertigo, and tinnitus, namely exploring the reason.
(2) Prescriptions are prescribed for treatment according to the pathogenesis and the patient's physical condition. In most cases, the brain is found to be slightly inflamed, and at this time, treatments against neuroinflammation are usually used.
(3) For the main direction of medication, if novel coronavirus remains in the body, antiviral drugs such as Paxlovid should be used as a priority. If there is no virus in the body, the drug is used from the perspective of reducing or eliminating the chronic inflammation of the patient, improving the metabolic circulation and immune mystery of patients. For example, rintatolimod (immunomodulator) and coenzyme Q10 + NADH (mitochondrial modulator) can be used to improve the immune system of patients.
(4) If Alzheimer 's disease are diagnosed, Lecanemab is needed to control the development of the disease. Eisai and Biogen announced that Lecanemab, an Alzheimer 's disease (AD) drug jointly developed by the two sides, has achieved good results in clinical trials for the treatment of patients with mild Alzheimer' s disease and Alzheimer 's disease, resulting in mild cognitive impairment (MCI).
(5) In case of psychiatric problems, a psychologist is needed. Massage of the brain can also be tried, and studies have shown that this is also beneficial for recovery.
6.How To Treat Long-Term COVID-19 Symptoms Of Dizziness From a Traditional Chinese Medicine(Tcm) Perspective?
From the theory of syndrome differentiation and treatment of TCM, the treatment of long-term COVID-19 symptoms of dizziness can obtain more accurate TCM syndrome differentiation and more suitable TCM formulas from the following three steps.
(1) Perform the observation, smelling, hearing, and inquiring of traditional Chinese medicine diagnosis, and consult the comprehensive physical examination report and four special examination reports of western medicine in the previous section at the same time. Only in this way can TCM doctors obtain the most detailed disease information of patients to support them to make the most accurate syndrome differentiation and treatment of patients' conditions.
(2) TCM doctors will classify and summarize the main symptoms, accompanying secondary symptoms, physical condition, and sick parts of the internal organs of the patients according to the most comprehensive disease information of the patients. First, the main symptoms are the most unbearable symptoms of patients at present, such as dizziness. Second, accompanying secondary symptoms are that suffered from the main symptoms, which means the patient is experiencing other uncomfortable symptoms, such as occasional chronic headache. Third, to find out the physical condition of the patient, which means the patient's current physical health status, belongs to which category in the TCM constitution. For example, yang-deficiency constitution, phlegm-dampness constitution, qi-deficiency constitution, blood stasis constitution, etc.
(3) TCM doctors, according to the above summary, combined with the internal organs and meridians related to symptoms, comprehensively use the theory and practical experience of TCM to make TCM prescriptions for patients. If acupuncture and moxibustion are required, these programs will also be prescribed.
Traditional Chinese medicine (TCM) theory is mainly based on: Zhang Zhongjing’s “Treatise on Febrile Diseases”, “Synopsis of Golden Chamber”, Huang Yuanyu's “Four Sacred Hearts Source”, “Typhoid Fever Suspension”, “Jinkui Suspension”, “Changsha Yao Jie”, Li Dongyuan 's “Treatise on the Spleen & Stomach”, and Zhang Jingyue' s “Jingyue Quanshu”.
TCM Practical experience, which can be found in Google Scholar (Fig. https://scholar.google.com/), and search for keywords for TCM treatment of long-term novel coronavirus symptoms. For example, COVID-19 Traditional Chinese Medicine, Long Covid Traditional Chinese Medicine. A large number of academic papers on medical research on the treatment of Long Covid by traditional Chinese medicine can be found in this way.
In order to make it easier for everyone to understand the treatment process of TCM, the following is a TCM treatment case of a patient with long-term COVID symptoms of dizziness.
Case 1:
Name: Chen, female, aged 51 years, height 161cm, weight 80 kg.
Medical History: PCR was positive for novel coronavirus on 17 April 2022, followed by typical symptoms of novel coronavirus infection: fever, cough, sore throat, sputum with blood streaks, ageusia, and anosmia. Two weeks later, the symptoms of novel coronavirus infection gradually relieved and disappeared. Later, dizziness symptoms appeared in succession.
Physical examination report of western medicine: (1) PCR test for novel coronavirus showed positive results again. (2) Cardiac examination showed arrhythmia. (3) Proinflammatory markers were high and there was slight systemic chronic inflammation. (4) Immune system examination items revealed abnormal lymphocyte subset determination, C-reactive protein, and immunoglobulin data.
Main symptoms: dizziness.
Accompanying secondary symptoms: occasional chronic headache.
Prescriptions given by Western physicians:
(1) Paxlovid (antiviral drug, use to prevent the replication of novel coronavirus in vivo).
(2) Coenzyme Q10 + NADH (mitochondrial modulator).
(3) rintatolimod (immunomodulator).
(4)Lecanemab, a new drug jointly developed by Eisai and Biogen, controls the development of the disease.
(5) Vitamin C, Vitamin D, Vitamin E, Sulforaphane and resveratrol. (Use to reduce the inflammatory reaction in vivo.)
TCM constitution: the body presents phlegm-dampness constitution and yang deficiency constitution.
TCM diagnosis evaluation: exogenous wind evil, Xifeng Tongluo, resulting in dizziness symptoms.
Prescription given by the TCM doctor:
(1) Banxia Tianma Pills are used to invigorate the spleen and removing dampness, reducing phlegm and wind, reduce dizziness symptoms.
(2) Mailuotong capsules are used to dredge meridian vascular congestion, protect cardiac pericardium and reduce arrhythmia.
(3) Qinggong Shoutao Pills are used to tonify the kidney and nourish yin and increase yang.
Acupuncture program given by the TCM: electricity is exerted to heat the moxibustion apparatus, and apply moxibustion at the following acupoints.
(1) Baihui, Ashi, Shenyu and Guanyuan points to improve brain metabolism.
7.Which Kind Of Health Products Are Beneficial To Improving Long-Term Covid-19 Symptoms Of Dizziness?
Taking the patient above as an example, we give the following health product recommendations based on her condition:
(1) Omega 3 (Ω3) fatty acids, containing high amounts of DHA and EPA, are used to improve brain function and protect against cardiovascular and cerebrovascular diseases.
(2) VC, VD and VE are used to scavenge free radicals, anti-oxidation, and reduce systemic chronic inflammation.
(3) Curcumin is used to scavenge free radicals, anti-oxidation, activate NRF2, and reduce systemic chronic inflammation.
(4) Sulforaphane is used to scavenge free radicals, anti-oxidation, activate NRF2, and reduce systemic chronic inflammation.
(5) American ginseng is sliced for making tea or taken American ginseng capsules to replenish qi.
8.What Exercises Are Beneficial To Improving Long-Term COVID-19 Symptoms Of Dizziness?
Taking the patient above as an example, we give the following exercise advice based on her condition:
(1)Do mindfulness meditation or Buddhist meditation.
(2)Enjoy the wild of natural oxygen bars, such as walking in the deep forest, and perform deep breathing exercises.
(3)Assist with head massage.
9.What Is Beneficial To Improving Long COVID Symptoms Of Dizziness And Vertigo In Terms Of Diet And Sleep?
Taking the patient above as an example, we give the following diet and sleep advice based on her condition:
(1) Control carbohydrate intake, which means reducing the amount of staple food such as rice and noodle, and control animal fat intake.
(2) Do not take any food after lunch, and have breakfast and lunch only a day. Losing weight at least more than 10% of body weight, which means losing 8 kg, reducing the degree of obesity.
(3) Bubble bathing until slightly sweating before sleeping, and lie in bed to do general muscle tightness and relaxation training, improving sleep quality.
10.Patients with dizziness and vertigo are welcome to contact with our Long Covid Health Center
If there are similar symptoms among readers, contact our Long COVID Care Center for assistance.
Phone: +852 5765 5768
Whatsapp: +852 5765 5768
WeChat: longcovidcarecenter
Email: support@longcovidcarecenter.org
【Disclaimer: The treatment of diseases is a very complex and professional affair. Due to the limitation, Long COVID Care Center can only carry out remote simple interviews, unable to face-to-face offline interviews and obtain comprehensive physical examination results. Therefore, the suggestions, guidance, protocols, and documents conveyed by Long COVID Care Center to patients can only be used as a reference for patients to understand their diseases in many aspects, but cannot be directly used as a treatment plan. Patients must discuss their symptoms with doctors in local hospitals through face-to-face communication. After the patients completed the physical examination required by doctors, they would get a prescription issued by doctors and get the treatment under the guidance of doctors. Therefore, Long COVID Care Center hereby declares that our center is completely exempted from liability when any adverse consequences are caused by self-treatment of the patient for applying any contents convoyed by the center, that is, we do not bear any responsibilities.】


